The International Tinnitus Journal
Official Journal of the Neurootological and Equilibriometric Society
Official Journal of the Brazil Federal District Otorhinolaryngologist Society
ISSN: 0946-5448

Google scholar citation report
Citations : 12717
The International Tinnitus Journal received 12717 citations as per google scholar report
The International Tinnitus Journal peer review process verified at publons
Indexed In
- Excerpta Medica
- Scimago
- SCOPUS
- Publons
- EMBASE
- Google Scholar
- Euro Pub
- CAS Source Index (CASSI)
- Index Medicus
- Medline
- PubMed
- UGC
- EBSCO
Volume 21, Issue 1 / June 2017
Research Paper Pages:30-34
Management of Benign Paroxysmal Positional Vertigo: A Comparative Study between Epleys Manouvre and Betahistine
Authors: Japneet Kaur, Karthik Shamanna
PDF
Abstract
Benign paroxysmal positional vertigo (BPPV) is the most common peripheral vestibular disorder, accounting for 20% of all vertigo cases. Idiopathic BPPV is most common between the ages of 50 and 70, although the condition is found in all age groups. This study was conducted in our institute on 90 patients who presented to the outpatient department with history of vertigo and were diagnosed with BPPV via a positive Dix Hallpike test. Patients were randomnly placed in three groups of 30 each. Patients in Group A were treated with Epleys manoeuvre alone, in Group B were treated with Epleys Manouvre followed by oral Betahistine and patients in Group C were treated with Betahistine alone. All the patients were followed up after 1 week and 4 weeks following treatment. In our study we found that patients responded better when they were treated with Epleys Manouvre with Betahistine with less relapse and recurrence. Treatment with Epleys manouvre resulted in early improvement of symptoms. It was found in our study that Betahistine as a sole modality of treatment of vertigo in BPPV can be preferred in patients who are unfit to undergo canal repositioning manouvres.
Keywords: benign paroxysmal positional vertigo, betahistine, dizziness
Introduction
Benign Paroxysmal Positional Vertigo (BPPV) is a common complaint of emergency department patients. Benign paroxysmal positional vertigo (BPPV) is the most common peripheral vestibular disorder, accounting for 20% of all vertigo cases [1-3]. Idiopathic BPPV is most common between the ages of 50 and 70, although the condition is found in all age groups. The incidence of idiopathic BPPV ranges from 11 to 64 per 100,000 per year Gender distribution is about equal for posttraumatic and post vestibular neuritis BPPV [4], although in its idiopathic form appears to be approximately twice as common in females [5]. BPPV was first described by Barany in 1921, and was later described in more detail by Dix and Hall pike in 1952 [6]. In Benign Paroxysmal Positional Vertigo patients typically complain of severe dizziness of sudden onset, lasting less than a minute on lying down or rising out of bed, rolling over, suddenly turning head to one side, bending forward and straightening, or by throwing head backwards to one side as when reaching for something or a shelf [7]. Although BPPV is incapacitating, it is a benign disease which usually has spontaneous remission within 4-6 months.
The importance of early diagnosis and treatment can lead to a much improved quality of life for patients afflicted by this ailment. BPPV can be diagnosed by Dix Hallpike test which can be performed in outpatient room [1]. In this test certain positions provoke movements of the particles within the affected semicircular canal leading to nystagmus, resulting nystagmus can indicate the canal affected.
In 1992, Epley first published his report on the canalolith repositioning procedure (CRP) [8]. Epley manoeuvre is effective in more than 90% of cases in eliminating BPPV [9]. Epleys manoeuvre is beneficial for treatment of BPPV by dislodging the otoconia in semicircular canals commonly posterior semicircular canal and reducing the symptoms. BPPV is highly amenable to treatment by particle repositioning manoeuvres and pharmacological therapy. In case of BPPV not responding to canal repositioning manoeuvres and pharmacotherap , surgery can be performed but it should be reserved for the most intractable or recurrent cases. Surgical procedures for intractable BPPV include Singular neurectomy proposed by Gacek and Posterior semicircular canal occlusion proposed by Money and Scott [10].
The purpose of this study was to compare the efficacy of three modalities of treatment, Epleys manoeuvre along with Betahistine, Betahistine alone and Epleys manoeuvre alone in patients who presented with vertigo to a tertiary care centre. Several studies have been conducted to evaluate the efficacy of Epleys manoeuvre in the treatment of BPPV proving the beneficial effects of Canal Repositioning Manouevre. It is done as an office procedure and includes putting the patient in certain positions in order to dislodge the otoconial debris responsible for the vertigo. It is a very safe and effective procedure with good results. However, in patients not fit for Canal Repositioning Manouevre, pharmacotherapy may be used as a modality of treatment.
Source of Data
A total of 90 Patients who presented to the ENT department with history of vertigo and were diagnosed to have BPPV via a Positive Dix Hallpike test were included in this study. The patients were randomized in three age and gender matched groups of 30 each. Group A received the Betahistine (16 mg) for 1 week followed by 1 month follow up, for patients in Group B canalith repositioning technique (Epleys manoeuvre) was done along with Betahistine (16 mg) therapy for 1 week, Group C patients were treated with Epleys manoeuvre alone.
Study period
October 2013 to September 2015
Study sample size
90 patients diagnosed with BPPV via positive Dix Hallpike were included in the study and it was carried out for the above mentioned time period.
Methodology for Data Collection
Data collection was started after obtaining clearance from the Ethics Committee. Informed consent for the study was obtained from all the patients who participated in this study. All the 90 patients in this study were evaluated before treatment with
1. Detailed history taking and clinical examination.
2. Subjective assessment of vertigo using:
a) Dizziness Handicap Inventory Questionnaire (DHI)
b) Visual Analogue Scale for Vertigo.
3. Dix Hallpike test
The patients were followed up weekly for 4 weeks to assess the efficacy of the treatment. The efficacy of the treatment was assessed using:
1. Subjective resolution of symptomatic vertigo on change in posture
2. Conversion of positive to negative Dix Hallpike
3. Frequency and severity of attacks of vertigo
4. Visual Analogue Scale for vertigo
5. DHI score for vertigo
SPSS v16.0 software was used to analyze the data obtained. Student t test (two tailed, independent) was used to find the significance of study parameters on continuous scale between two groups (Inter group analysis on metric parameters). Student t test (two tailed, dependent) was used to find the significance of study parameters on continuous scale within each group. Chi square/ Fisher Exact test was used to find the significance of study parameters on categorical scale between two or more groups. McNemar test was used to find the significance of change in each for pre and post treatment.
Inclusion criteria:
1. Subject who was >18 years of age < 60 years.
2. Strong history suggestive of BPPV.
3. Subject with positive findings of vertigo and nystagmus when the DixHallpike manoeuvre was performed during examination. A DixHallpike manoeuvre was considered positive when the patient experienced nystagmus but resolved or fatigued in less than 60 seconds.
Exclusion criteria:
1. Subjects who were unable to ambulate.
2. Subjects with severe cervical spine disease
3. Subjects with known cerebral vascular disease like carotid stenosis
4. Subjects with a known history of Meniere’s disease.
5. Subjects with h/o cardiac complaints
6. Subjects with vertigo due to central causes.
Results
The age of the patients included in this study ranged from 20 to 60 years. The sample population was gender matched. All the 90 patients had sudden onset of the symptoms of vertigo. Amongst the study population 47 were males and 43 were females. In the Epleys manoeuvre with Betahistine group, 23 (76.7%) patients had duration of vertigo less than 10 days, while 7 (23.2%) patients, had vertigo for more than 10 days. In the Betahistine alone group, 26 (86.7%) patients had less than 10 days of vertigo, while 3 (10%) patients had more than 10 days of vertigo. In the Epleys alone group, 24 (80%) patients had vertigo of less than 10 days, while 6 (20%) patients had vertigo of more than 10 days. Overall, majority of patients in both the groups had less than 10 days history of vertigo
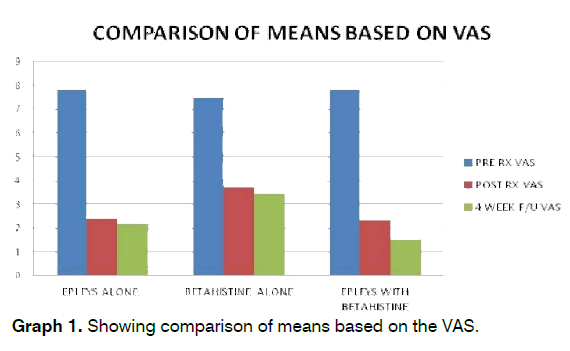
On analysing the results from the Visual Analogue Scale, in the Epleys alone group, the Mean pretreatment VAS score was 7.8 ± 0.942, the mean post treatment VAS score was 2.40 ± 1.28 at the end of 1 week and 2.17±1.28 at end of 4 weeks. This difference was statistically significant with a P value of 0.001. In the Epleys with Betahistine group, the Mean pretreatment VAS score was 7.77 ± 0.90, the mean post treatment VAS score was 2.33 ± 1.35 at the end of 1 week and 1.5 ± 0.63 at end of 4 weeks. This difference was statistically significant with a P value of 0.001. In the Betahistine alone group, the Mean pretreatment VAS score was 7.47 ± 0.973, the mean post treatment VAS score was at the end of 1 week and 3.47 ± 1.82 at end of 4 weeks. This difference was statistically significant with a P value of 0.001. At the end of 1 week, the mean post treatment VAS score was compared between Epleys with Betahistine group (2.33 ± 1.35) and Betahistine alone group (3.73 ± 1.95). This was found to be strongly statistically significant with a P value of 0.002. The mean post treatment VAS score was compared between Epleys with Betahistine group and Epleys alone group was found to be strongly statistically significant with a P value of 0.001. At the end of 4 weeks, the mean post treatment VAS score of Epleys alone group, Epleys with Betahistine group and that of Betahistine alone group was found to be statistically significant with a P value of 0.001(Graph 1).
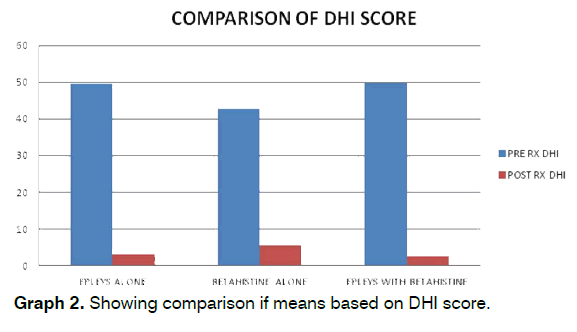
All the patients had DHI score in the range of 32-56, suggestive of moderate vertigo (Graph 2). It was observed that at the end of four weeks, there was significant change in the pretreatment and post treatment DHI scores in the three groups (p < 0.001). There was no worsening of the vertigo observed in the groups during the study period. In the Epleys with Betahistine group 1 patient did not improve with treatment at the end of 1 week. In the Betahistine only group 2 patients did not respond to treatment at 1 week and 1 patient did respond at 4 weeks and was termed as non-responder. 1 patient had recurrence of symptoms at 4 weeks after initial improvement and was termed as relapse. In the Epleys only group 1 patient was a nonresponder and 1 patient had relapse of vertigo at the end of 4 weeks.
In our study the patients were assessed by a Visual Analogue Scale for severity of vertigo. The patients were asked to scale their symptoms of vertigo from 0 to 10, where 0 was no vertigo. The grading was 1-4 mild vertigo, 4-8 moderate and 8-10 was severe vertigo. The improvement in post treatment Visual Analogue Scale in the Epleys with Betahistine group was better than the Betahistine group alone, with a significant p value of 0.002. In our study, treatment with Epleys and Betahistine showed better improvement in the mean VAS score at 1 and 4 weekly follow-up. There was higher percentage of improvement in mean post treatment VAS score seen in the Epleys with Betahistine group as compared to the Betahistine alone group. In our study there was no statistically significant difference in the post treatment DHI score between the two groups. However, the difference between the pre and post treatment DHI score was strongly statistically significant with a p value of < 0.001 in each group. Patients in both the groups showed significant improvement in symptoms like vertigo on looking up, while tying shoes, vertigo on turning in the bed, vertigo on bending over and other daily activities. The Epleys with Betahistine group showed higher percentage of improvement (94.8%) in symptoms as compared to the Betahistine alone group (87.1%). The patients in the Epleys with Betahistine group showed earlier resolution of vertigo within first 2 days of the treatment. These patients had longer relief of symptoms and no relapse or recurrence. The patients in the Betahistine alone group showed improvement of symptoms from day 4 or day 5 of starting the treatment. Patients who were treated with Epleys manoeuvre alone showed resolution of vertigo in the first 2 days but showed relapse of symptoms. There was no worsening of the vertigo in both the groups during the study period.
Discussion
Current modalities of treatment for BPPV include various vestibular rehabilitation exercises, pharmacological drugs and surgery in resistant cases. This study was conducted on 3 groups of patients presenting with BPPV, where one group was treated with Epleys manoeuvre along with pharmacological therapy (Betahistine) and the other group was treated with pharmacological drug (Betahistine) only and the third group was treated with Epleys manoeuvre alone The effectiveness of treatment in all the three groups was evaluated and compared based on the symptomatologic improvement, visual analogue scale and DHI scores.
In a study conducted by Epley in 1992, he studied 30 patients with BPPV. He conducted Epleys exercise on the patients with positive Dix hallpike test and followed them after 1 week. There was 90% cure rate seen after Epleys manoeuvre [11]. Similar study was conducted by Parnes and Price in 1993 on 38 patients with BPPV based on positive Dix hallpike test and symptoms of BPPV. They followed up the patients after 3-4 weeks of performing Epleys manoeuvre and observed a cure rate of 68.5% [3].
Hardman et al. found a cure rate of 57%, in a group of 30 patients who were treated by Epleys manoeuvre. In this study, 33% patients showed improvement while 10% had no change in the symptoms [12]. Betahistine dichloride is a histamine analogue used in the treatment of vertigo, motion sickness, and various vestibular disorders of peripheral and central origin. Betahistine acts on H3 and H1 receptors. It causes vasodilation of blood vessels in the inner ear leading to improvement of microcirculation in the labyrinth.
According to a study done by Katerina Stambolieva et al., treatment with Betahistine dihydrochloride helped to restore the postural stability in patients who were treated with Betahistine and canal repositioning manoeuvres. Ten days after treatment with Betahistine it was noted that the Sway Velocity was normalized and did not differ from that in healthy subjects. In their study, therapy with Betahistine dihydrochloride used after applying Semont liberatory manoeuvre and Brandt Daroff exercises showed better results evaluated by Epley criteria 14 days after treatment, independently of age of patients with a significant difference (p < 0.01) [13].
In our study, treatment with Epleys and Betahistine showed better improvement in the mean VAS score at 1 and 4 weekly follow-up. There was higher percentage of improvement in mean post treatment VAS score seen in the Epleys with Betahistine group and Epleys group as compared to the Betahistine alone group.
According to Katherine et al. long presence of otoconias in the lumen or in the cupula of the semicircular canal permanently damaged the normal function of motion sensitive hairs cells in the inner ear, because of that the therapy with Epleys Manouvre and with Betahistine dihydrochloride 20 days after Epleys Manouevre have a weak effect on the postural stability of patients with duration of BPPV above 60 days. It was suggested that long lasting abnormality in the peripheral vestibular system activates certain adaptation processes in central nervous system connected with mechanisms participating in the maintenance of posture and take a form of new pattern of postural stability in patients with duration of BPPV above 60 days, and the treatment with Betahistine dihydrochloride after Epleys Manouevre is not effective.
For the other group of patients (less than 60 day duration of BPPV) the treatment with Betahistine dihydrochloride after Epleys Manouevre was effective and ten days after treatment postural stability of patients was normalized. Thus the study concluded that Betahistine dihydrochloride accelerates the recovery of function of vestibular system, by improving blood flow in the inner ear and normalization of the function of motion sensitive hair cells is faster. In a study conducted by Cavaliere et al. comparing two physical manouvres with and without betahisitine, the group treated with betahistine showed better improvement as compared to physical therapy alone group [14].
In our study greater improvement was seen in the group receiving Epleys with medication therapy. Thus, the cumulative effect of particle repositioning and pharmacotherapy was statistically significant. Patients had faster recovery, lesser recurrence and longer relief of symptoms.
Conclusion
Benign paroxysmal positional vertigo is an incapacitating condition which is self-remitting but can recur. It is diagnosed by Dix Hallpike test, which is an easy test performed in outpatient room. Patients should be reassured about the benign nature of the condition and the possible treatment options. Amongst the various vestibular rehabilatation exercices for the treatment of Benign Paroxysmal Positional Vertigo, Epleys manouevre has been found to be highly safe and effective and quick procedure. Our study concludes that, Epleys with Betahistine is effective in management of patients of BPPV and it is helpful in bringing their symptoms to tolerable level. Pharmacological therapy with Betahistine when used in conjunction with Epleys is a safe modality of treatment. Betahistine can be used as a sole modality of treatment in patients of BPPV who are unfit to undergo canalolith repositioning manoeuvres. It provides short term relief for acute symptoms associated with BPPV by improving the microcirculation in the labyrinth and reducing the symptoms of vertigo. There may be relapse of symptoms when used alone without Canal Repositioning Manouvre.
References
- Bhattacharyya N, Baugh RF, Orvidas L, Barrs D, Bronston L, Cass S, et al. Clinical practice guideline:benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg. 2008;139(5):S47-81.
- Froehling DA, Bowen JM, Mohr DN, Brey RH, Beatty CW, Wollan PC, et al. The canalith repositioning procedure for the treatment of benign paroxysmal positional vertigo: a randomized controlled trial. Mayo Clin Proc. 2000;75(7):695-700.
- Parnes LS, Agrawal SK, Atlas J. Diagnosis and management of benign paroxysmal positional vertigo (BPPV). CMAJ. 2013;169(7):681-93.
- Hilton MP, Pinder DK. The Epley (canalith repositioning) manoeuvre for benign paroxysmal positional vertigo. Cochrane Database Syst Rev. 2004;(2):CD003162.
- Baloh RW, Honrubia V, Jacobson K. Benign positional vertigo: clinical and oculographic features in 240 cases. Neurology 1987;37(3):371-8.
- Sjoback DG, Andersen RH. Pathology of the vestibular system: Scott Brown’s Textbook of Otorhinolaryngology and Head and Neck Surgery,7th ed. Great Britain: Hodder Arnold Ltd; 2008. p.367-8.
- Dix MR, Hallpike CS. Pathology, symptomatology and diagnosis of certain disorders of the vestibular system. Proc R Soc Med. 1952;45(6):341-54.
- Epley JM. The canalith repositioning procedure for treatment of benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg.1992;107(3):399-404.
- Benjamin T, Crane DA. Schessel Chapter 165 Peripheral Vestibular DisordersIn: Cummins C W, Flint P W. Cumming’s Otolaryngology, Head and neck surgery. 5th ed. Volume 1: Philadelphia USA: Elsevier; 2007. p.23-31.
- Parnes LS, Aggrawal SK. Peripheral audiovestibular disorders: Brackmann neurotology:2nd ed. 2005 by Mosby, Inc:p.652.
- Epley JM (1992) The canalith repositioning procedure: for treatment of benign paroxysmal positioning vertigo. Otolaryngol Head Neck Surg. 1992;10:299-304.
- Herdman J, Tuss JR. Assessment and treatment of patients with Benign Paroxysmal Positional Vertigo. In Herdman SJ. Vestibular Rehabilitation 2nd ed. Davis FA Company Philadelphia 2000;451-75.
- Stambolieva K, Angov G. Effect of treatment with betahistine dihydrochloride on the postural stability in patients with different duration of benign paroxysmal positional vertigo. Int Tinnitus J. 2010;16(1):32-6.
- Cavaliere M, Mottola G, Iemma M. Benign paroxysmal positional vertigo: a study of two manoeuvres with and without betahistine. Acta Otorhinolaryngol Ital. 2005; 25(2):107-12.
References
1Senior Resident, Department of Otolaryngology, GGS Medical College, Faridkot
2Associate Professor, Department of Otolaryngology, Bangalore Medical College and Research Institute
Institution: Bangalore Medical College and Research Institute
Send correspondence to:
Japneet Kaur MD
H.I.G 202 Sector 71, Mohali, Punjab 160071, India E-mail: drjapneetkaur@gmail.com
Paper submitted to the ITJ-EM (Editorial Manager System) on February 01, 2017; and accepted on March 29, 2017.
Citation: Kaur J, Shamanna K. Management of Benign Paroxysmal Positional Vertigo: A Comparative Study between Epleys Manouvre and Betahistine. Int Tinnitus J. 2017; 21(1): 30-34