The International Tinnitus Journal
Official Journal of the Neurootological and Equilibriometric Society
Official Journal of the Brazil Federal District Otorhinolaryngologist Society
ISSN: 0946-5448

Google scholar citation report
Citations : 12717
The International Tinnitus Journal received 12717 citations as per google scholar report
The International Tinnitus Journal peer review process verified at publons
Indexed In
- Excerpta Medica
- Scimago
- SCOPUS
- Publons
- EMBASE
- Google Scholar
- Euro Pub
- CAS Source Index (CASSI)
- Index Medicus
- Medline
- PubMed
- UGC
- EBSCO
Volume 24, Issue 2 / December 2020
Research Article Pages:49-53
10.5935/0946-5448.20200009
Somatosensory-Auditory Processing of the Fifth Cervical Nerve in Tinnitus
Authors: Henk M Koning
PDF
Abstract
Introduction: Cervical spinal nerve projections influence auditory responses and play a role in the pathology of tinnitus.
Objectives: The intention of our research was to lay down the amenity of treatment of the fifth (C5) cervical nerve to lessen tinnitus and to obtain specifications associated with a long-term effect of this method.
Design: Subjects were 54 tinnitus patients who were treated with infiltration of the fifth cervical nerve. Clinical data form these patients were reviewed retrospectively. An independent perceiver evaluated the long-term effect of the therapy by telephone interview.
Results: Treating the C5 is beneficial for 30% of the tinnitus patients. The majority of patients with a beneficial result rated the tinnitus reduction of 50% or more. At 9 months, half of the patients still had benefit. Less hearing at 1 kHz together with a large spur in front of the fifth cervical vertebrae forecasted a beneficial effect of the C5 therapy on tinnitus at 7 weeks.
Conclusions: Treating cervical spine complaints can lessen tinnitus. Therapy of C5 resulted in less tinnitus for 30% of the tinnitus patients. However, selection of tinnitus patients with an evident spur in front of the fifth cervical vertebrae together with a less hearing at 1 kHz will improve the success rate of C5 therapy mp3download.link Best YouTube to MP3 converter. Download MP3 from YouTube for Free. one would honestly have expected more on the track mp3-go.net Download Mp3 songs for free Given the legendary pedigree of the man behind the sound downloadmp3-gratis.biz Download mp3 songs online at Mp3 Converter, watch high quality online music videos download-mp3gratis.me watch and download free songs of the highest quality. Listen to songs online here comfortably without any annoying advertisements. metrolagu.com Easy to use and free MP3 downloader. YouTube To MP3 download in seconds using the best YouTube to MP3 converter. YouTube Mp3 Get the latest song by simply typing the latest artist or song title in the Search menu. Mp3 file format with 128 - 320 Kbps bitrate converted from YouTube videos. read at this blog All those artist performances are still available on YouTube today find more here
Keywords: Tinnitus, nerve root infiltration, cochlear nucleus, cervical spine, fifth cervical nerve, cuneate nucleus, hearing loss
Introduction
Tinnitus is typified by neural hyperactivity in the central auditory network caused by the input of the somatosensory and auditory nerves [1]. Hyperactivity of the auditory nuclei may develop after auditory nerve injury and from somatosensory insults caused by cervical pathology [2,3]. Also, diminished auditory input can reinforce the somatosensory influence on auditory neurons4. Therefore, hearing loss can increase the risk that cervical pathology can generate tinnitus. Cervical spinal nerve projections influence auditory responses and play a role in the pathology of tinnitus. The proper selection for which cervical nerve is involved in each individual tinnitus patient is difficult and further studies are needed. The intention of our research was to lay down the amenity of treatment of the fifth (C5) cervical nerve to lessen tinnitus and to obtain specifications associated with a long-term effect of this method.
Materials and Methods
The Medical Ethics Committees United (Nieuwegein, the Netherlands) validated the analysis. All patients who underwent therapy of C5 in a three years interval (2016 - 2019) participated in the study.
Therapy of C5: A needle (Top Neuropole needle XES, Tokyo, Japan) was set in the foramen between the fourth and the fifth cervical vertebrae. If the needle was at the appropriate position and no blood was aspired a mix of one millilitre bupivacaine 0.5% (Bupivacaine Aurobindo, Baarn, the Netherlands) with twenty milligram dexamethasone (Dexamethasone CF, Etten-Leur, the Netherlands) was applied. The patients were assessed again 7 weeks postoperative.
Data Assessment: Information from patient charts were written down, together with the self-reported improvement at seven weeks postoperative on a four-point Likert scale (none [0%], slight [less than 25%], moderate [25% to 50%], good [50% or more]), and the duration of relief. Successfully treated patients without a reported relapse were evaluated by telephone interview to assess the time of relief
Statistical Methods: Data were processed using Minitab 18 (Minitab Inc., State College, PA, USA). Survival analysis techniques were used to determine the time of relief following treatment. Multiple regression analysis helped us to forecast a beneficial result of the therapy.
Results
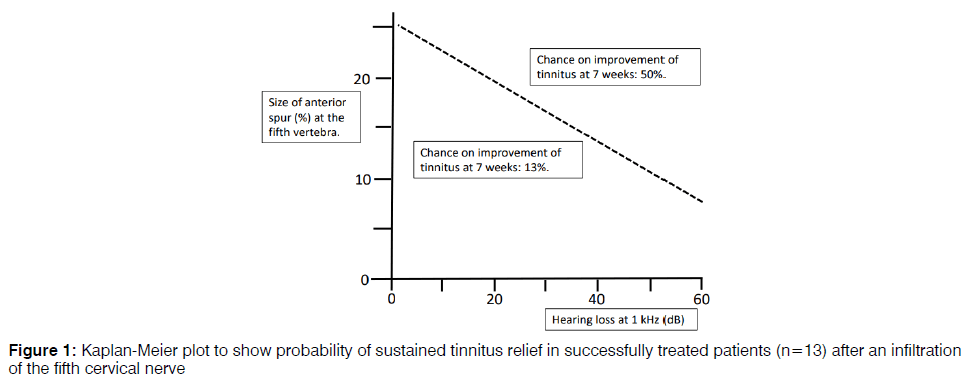
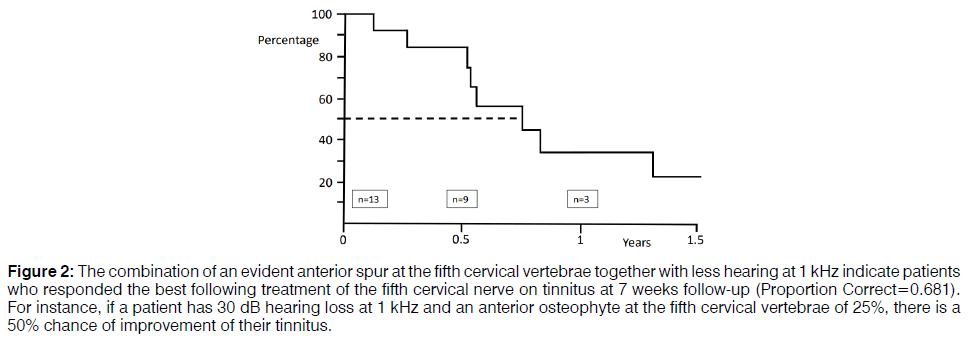
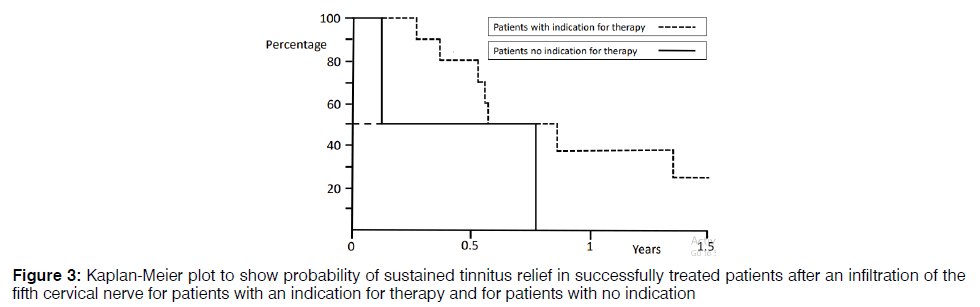
In a three-year period, 54 patients underwent a procedure of the C5 to treat their tinnitus. The aspects of the patients are recognizable in Table 1. On follow-up, sixteen patients (30%) had less tinnitus. The successfully treated patients evaluated the quantity of relief from their tinnitus (63% good, and 37% moderate). Unfavourable events of the nerve root infiltration of the C5 were reported in two patients (4%). One patient (2%) reported an aggravation of their tinnitus and one patient (2%) reported dizziness (1%) following the treatment. Figure 1 manifests a Kaplan– Meier plot demonstrating the possibility of enduring effect after beneficial C5 therapy. At 9 months, 50% of these patients still had benefit. Patients with a beneficial result of C5 therapy at follow-up were set side by side with the ones who had no effect (Table 2). Hearing loss at 1 kHz and 2 kHz, and a larger anterior cervical spur at C5 were associated with a beneficial effect of C5 therapy on tinnitus, however it did not reach statistical significance. Multivariate statistics qualified that less hearing at 1 kHz together with the dimension of the spur in front of the fifth cervical vertebrae forecasted a beneficial effect of the C5 therapy on tinnitus at 7 weeks. In Figure 2 the tinnitus patients with more prospect for a beneficial C5 therapy are indicated. With this indication there is a sensitivity of 80% and a specificity of 63% to prognosticate an advantageous C5 therapy for tinnitus. Positive and negative predictive values are 50% and 86% respectively. Patients with this indication had a better result of therapy (good for 67% compared to good for 33% with no indication; p=0.292) and a longer period of relief (Figure 3).
| Prevalence | Median | Q1 – Q3 | |
|---|---|---|---|
| Age (year) | 57.5 | 50.8 – 65.3 | |
| Gender (male) | 65% | ||
| Unilateral tinnitus | 35% | ||
| Self-perceived hearing loss | 67% | ||
| Cervical pain | 76% | ||
| Period of tinnitus (year) | 4.0 | 1.4 – 16.0 | |
| Hearing loss (dB) at: | |||
| 250 Hz | 15 | 10 – 30 | |
| 500 Hz | 15 | 10 – 30 | |
| 1 KHz | 15 | 10 – 40 | |
| 2 KHz | 25 | 10 – 40 | |
| 4 KHz | 40 | 23 – 55 | |
| 8 KHz | 48 | 26 – 70 |
Table 1: Clinical Characteristics of the patients with tinnitus.
| Positive effect of therapy of nerve C5 (n=16) | No effect of therapy of nerve C5 (n=38) | P-value | |||||
|---|---|---|---|---|---|---|---|
| Prev. | Mean | SEM | Prev. | Mean | SEM | ||
| Gender (male) | 63% | 66% | 0.818 | ||||
| Unilateral tinnitus | 25% | 39% | 0.301 | ||||
| Self-perceived hearing loss | 75% | 63% | 0.392 | ||||
| Cervical pain | 88% | 71% | 0.177 | ||||
| Age at the start of tinnitus (year) | 42 | 4.0 | 49 | 2.1 | 0.121 | ||
| Hearing loss (dB) at: | |||||||
| 250 Hz | 25 | 5.7 | 21 | 3.4 | 0.478 | ||
| 500 Hz | 27 | 5.7 | 21 | 3.3 | 0.301 | ||
| 1 KHz | 31 | 5.6 | 21 | 3.6 | 0.152 | ||
| 2 KHz | 33 | 4.8 | 25 | 3.2 | 0.168 | ||
| 4 KHz | 40 | 5.1 | 42 | 4.0 | 0.785 | ||
| 8 KHz | 48 | 6.7 | 48 | 4.3 | 0.965 | ||
| Angle between vertebrae C2 and C6 (degrees): | 4.8 | 3.3 | 7.3 | 1.7 | 0.520 | ||
| Farfan’s measurement of disc space height (%): | |||||||
| • C2-C3 | 41 | 1.5 | 39 | 1.4 | 0.336 | ||
| • C3-C4 | 34 | 2.9 | 35 | 1.8 | 0.732 | ||
| • C4-C5 | 35 | 2.4 | 33 | 1.8 | 0.474 | ||
| • C5-C6 | 28 | 2.3 | 28 | 1.7 | 0.992 | ||
| • C6-C7 | 28 | 2.4 | 27 | 1.8 | 0.780 | ||
| Size of anterior osteophyte (%) at: | |||||||
| • C3 | 7 | 1.7 | 6 | 1.0 | 0.816 | ||
| • C4 | 10 | 1.3 | 12 | 1.6 | 0.289 | ||
| • C5 | 20 | 2.1 | 15 | 1.4 | 0.100 | ||
| • C6 | 14 | 1.9 | 13 | 1.1 | 0.592 | ||
Table 2: Patients with a positive effect of therapy of the C5 nerve root on their tinnitus at 7 weeks were compared with non-responders.
Figure 2: The combination of an evident anterior spur at the fifth cervical vertebrae together with less hearing at 1 kHz indicate patients who responded the best following treatment of the fifth cervical nerve on tinnitus at 7 weeks follow-up (Proportion Correct=0.681). For instance, if a patient has 30 dB hearing loss at 1 kHz and an anterior osteophyte at the fifth cervical vertebrae of 25%, there is a 50% chance of improvement of their tinnitus.
Discussion
Treating the C5 is beneficial for 30% of the tinnitus patients. The majority of patients with a beneficial result rated the tinnitus reduction of 50% or more. At 9 months, half of the patients still had benefit. Less hearing at 1 kHz together with a large spur in front of the fifth cervical vertebrae forecasted a beneficial effect of the C5 therapy on tinnitus at 7 weeks. Afferent cervical nerves, especially from the nerves C2, C7, and C8, influence auditory responses2. However, other cervical nerves could also be related to the pathogenesis of tinnitus and might be an option for therapy of tinnitus. We found that therapy of C5 could reduce tinnitus in 30% of the tinnitus patients. Compared to the prevalence of C2 (25%) [5], C3 and C4 (19%) [6], and C8 (26%) [7] in a cohort of tinnitus patients, C5 plays an important role in the pathogenesis of tinnitus. Tinnitus may be related to hyperactivity in central auditory network [4-8]. The heightened spontaneous rates of neurons could be caused by reduced inhibition of the fusiform cells, more excitability of the fusiform cells, or more excitation of the cochlear nucleus from the somatosensory nervous system [9]. Noise-induced injury to inner hair cells raises the spontaneous firing rate of neurons in several auditory structures [10]. Even with hearing thresholds in the clinically normal range (i.e. less than 20 decibel hearing loss) there is evidence for cochlear lesions, outer hair cell injury, or threshold elevations in patients with tinnitus [11]. In our study, hearing loss at 1 kHz and a large anterior spur at C5 seems to be responsible for inducing the hyperactivity of the auditory system by cervical nerve C5. Tinnitus can be caused by degeneration of the cervical discs [12]. Somatosensory input from the cervical spine can induce aberrant neuronal activity in central auditory pathways, which may be recognized as tinnitus [13]. The size of the anterior spur of the vertebra seems the most prominent sign of cervical disc degeneration associated with to tinnitus6. The location of the spur in front of the vertebra indicates which cervical nerve is involved. A spur in front at the third cervical vertebrae might provoke C3 and C4, while a spur in front of the fifth cervical vertebrae can do the same for C5. Auditory-somatosensory integration occurs in auditory nuclei [4-14]. Alterations of either the somatosensory or auditory input lead to compensatory shifts in the balance of excitation and inhibition in the central auditory network [2]. This imbalance is seen in the upregulation of somatosensory input after reduced auditory input, the increased sensitivity of auditory neurons for somatosensory stimuli, and, as end result, more spontaneous firing of a confined group of neurons that are innervated by those somatosensory inputs [2-9]. Already for the upper cervical nerves, auditory-somatosensory integration was observed in tinnitus patients. The magnitude of the spur in front of the third cervical vertebrae combined with the hearing loss at 2 kHz specify the tinnitus patients who may profit of therapy of the C3 and C4. In the present study, we found a similar combination of signs of cervical degeneration and hearing loss at specific frequency in tinnitus patients responding to therapy of C5.
Conclusion
This study has some limitations which could be addressed in future studies. The retrospective implementation, selfreported treatment and outcome estimations, and the total patients are subject of discussion. In future studies, researchers should focus on a prospective study with more patients and a clear patient selection, based on the diagnostic criteria described in this study. Treating cervical spine complaints can lessen tinnitus. Therapy of C5 resulted in less tinnitus for 30% of the tinnitus patients. However, selection of tinnitus patients with an evident spur in front of the fifth cervical vertebrae together with a less hearing at 1 kHz will improve the success rate of C5 therapy.
Conflict of Interest
The authors declare no potential conflict of interest on publishing this paper.
References
- Zeng C, Yang Z, Shreve L, Bledsoe S, Shore S. Somatosensory projections to cochlear nucleus are upregulated after unilateral deafness. J Neurosci. 2012;32:15791-801.
- Dehmel S, Cui YL, Shore SE. Cross-modal interactions of auditory and somatic inputs in` the brainstem and midbrain and their imbalance in tinnitus and deafness. Am J Audiol. 2008;17:193-209.
- Bressi F, Casale M, Papalia R, Moffa A, Di Martino A, Miccinilli S, et al. Cervical spine disorders and its association with tinnitus: The "triple" hypothesis. Med Hypotheses. 2017;98:2-4.
- Wu C, Stefanescu RA, Martel DT, Shore SE. Tinnitus: Maladaptive auditory-somatosensory plasticity. Hear Res. 2016;334:20-9.
- Koning HM, Ter Meulen BC. Pulsed radiofrequency of C2 dorsal root ganglion in patients with tinnitus. Int Tinnitus J. 2019;23:91-96.
- Koning HM. Upper Cervical Nerves Can Induce Tinnitus. Int Tinnitus J. 2020;24:26-30.
- Koning HM, Ter Meulen BC. The eight cervical nerve and its role in tinnitus. Int Tinnitus J. 2020;24:15-20.
- Robertson D, Bester C, Vogler D, Mulders WH. Spontaneous hyperactivity in the auditory midbrain: relationship to afferent input. Hear Res. 2013;295:124-9.
- Shore SE. Plasticity of somatosensory inputs to the cochlear nucleus implications for tinnitus. Hear Res. 2011;281:38-46.
- Manohar S, Dahar K, Adler HJ, Dalian D, Salvi R. Noise-induced hearing loss: Neuropathic pain via Ntrk1 signalling. Mol Cell Neurosci. 2016;75:101-12.
- Roberts LE, Eggermont JJ, Caspary DM, Shore SE, Melcher JR, Kaltenbach JA. Ringing Ears: The Neuroscience of Tinnitus. J Neurosci. 2010;30:14972-9.
- Montazem A. Secondary Tinnitus as a Symptom of Instability of the Upper Cervical Spine: Operative Management. Int Tinnitus J. 2000;6:130-3.
- Shore S, Zhou J, Koehler S. Neural mechanisms underlying somatic tinnitus. Prog Brain Res. 2007;166:107-23.
- Basura GJ, Koehler SD, Shore SE. Multi-sensory integration in brainstem and auditory cortex. Brain Res. 2012;1485:95-107.
Department of Pain therapy, Pain Clinic De Bilt, De Bilt, The Netherlands, E-mail: hmkoning@pijnkliniekdebilt.nl
Send correspondence to:
Henk M Koning
Department of Pain therapy, Pain Clinic De Bilt, De Bilt, The Netherlands, E-mail: hmkoning@pijnkliniekdebilt.nl
Phone: +0031302040753
Paper submitted on July 07, 2020; and Accepted on July 18, 2020
Citation: Somatosensory-Auditory Processing of the Fifth Cervical Nerve in Tinnitus. 24(2):47-51.